For many individuals, dry eye disease is an ongoing struggle marked by irritation, burning, watery eyes, and inconsistent vision. While over-the-counter drops may offer short-term relief, they often fail to provide lasting hydration. In many cases, the issue isn’t a lack of tear production - it’s that tears drain away too quickly.
One innovative option designed to provide longer-term relief is LACRIFILL®, a modern approach to punctal occlusion that helps preserve your natural tears and restore balance to the ocular surface.
What Is LACRIFILL® Canalicular Gel?
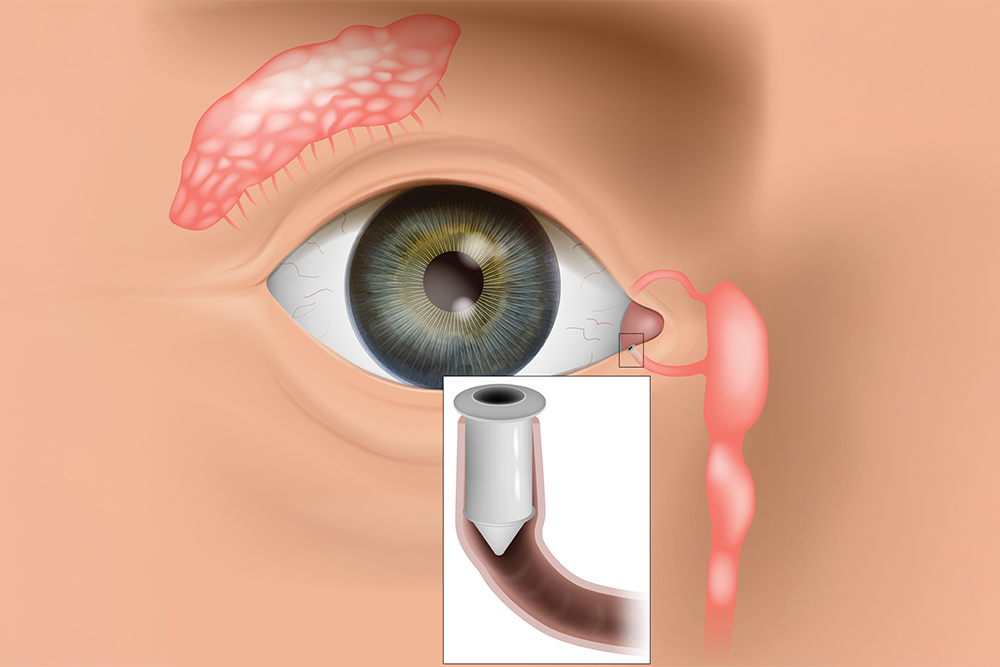
LACRIFILL® is a soft, clear gel that is placed inside the eye’s natural tear drainage channels, known as the canaliculi. These tiny channels are responsible for carrying tears away from the surface of the eye and into the nasal cavity.
For individuals with dry eye disease, tears often drain away too quickly. When this happens, the eye does not stay properly lubricated, leading to dryness and irritation. LACRIFILL® works by gently filling part of the drainage pathway, slowing tear outflow so that your natural tears remain on the eye longer.
Unlike traditional artificial tears that supplement moisture from the outside, LACRIFILL® helps you retain the tears your body already produces. This treatment is FDA-cleared and has been clinically studied for safety and effectiveness in managing dry eye symptoms.
How Does LACRIFILL® Work?
Every time you blink, a thin layer of tears spreads across the surface of your eye. This tear film keeps your eyes smooth, hydrated, and protected from debris and infection. After serving their purpose, tears drain through small openings in the inner corners of the eyelids (called puncta), passing into the canaliculi and eventually into the nose. In dry eye patients, this drainage process may occur too rapidly, leaving the surface of the eye exposed and under-lubricated.
LACRIFILL® forms a soft gel barrier within the drainage system, reducing tear loss and improving moisture retention. By keeping tears on the eye longer, it supports a healthier tear film and enhances overall comfort.
The gel gradually biodegrades over time and is naturally reabsorbed by the body. Relief typically lasts several months, and the treatment can be repeated when necessary.
Benefits of LACRIFILL®
LACRIFILL® offers several advantages for patients struggling with persistent dry eye symptoms:
FDA-cleared and clinically evaluated for safety and performance
Quick, non-surgical procedure performed in-office
No downtime or recovery period required
Preserves your body’s natural tears rather than relying solely on artificial drops
Provides extended relief that can last for months
Biocompatible material designed to work harmoniously with the body
Customizable treatment approach based on your individual tear drainage system
For patients who are tired of frequent eye drop use, this longer-lasting solution can be life-changing.

Dry eye is a common condition that occurs when your eyes do not produce enough tears or when the tears evaporate too quickly. This can result in discomfort, irritation, and a gritty sensation in the eyes. Understanding the causes and symptoms of dry eye is crucial for finding effective treatment options. Tyrvaya offers a breakthrough solution for dry eye relief.
What Causes Dry Eye?
There are several factors that can contribute to the development of dry eye. The meibomian glands are responsible for producing the oily component of the tear film, which helps prevent evaporation of tears and maintains a smooth ocular surface. Meibomian gland dysfunction occurs when these glands become blocked, leading to a decrease in the quantity and quality of the meibum. This can result in evaporative dry eye, discomfort, and inflammation of the eyelid margins.
Another common causes is age. As we get older, our tear production tends to decrease, making us more prone to dryness. Hormonal changes, such as those that occur during menopause, can also affect tear production and lead to dry eye.
Environmental factors can play a role as well. Dry or windy climates, air conditioning, and excessive screen time can all contribute to dry eye. Additionally, certain medications, such as antihistamines and antidepressants, can cause dryness as a side effect.
Other underlying health conditions, such as autoimmune diseases like Sjogren's syndrome or rheumatoid arthritis, can also contribute to dry eye. In these cases, the body's immune system mistakenly attacks the tear glands, leading to reduced tear production.

Optomap is an innovative new technology that gives eye doctors the ability to perform ultra-wide retinal imaging that is far superior to what can currently be achieved using conventional retinal imaging options. In contrast to conventional retinal imaging, Optomap captures at least 50% more of the retina in a single capture, and with Optomap’s multi-capture function, up to 97% of the retina can be viewed. This gives eye care professionals greater opportunity to monitor the health and condition of patient vision.
Why is Optomap important?
Optomap is another great preventative eyecare technology tool. By allowing your eye doctor to have a comprehensive view of your retina, they will be able to detect any developing eye diseases early on, before they have a detrimental impact on your vision and day to day life. Not only can Optomap detect eye conditions such as retinal holes, retinal detachment, macular degeneration and diabetic retinopathy, but it can also be used to identify some general health conditions such as cardiovascular disease, stroke and cancer.

Medical eye exams are comprehensive evaluations of the health and function of the eyes, essential for maintaining optimal vision and preventing potential eye conditions. Regular medical eye exams are fundamental for proactive eye health management and ensuring ongoing visual wellness.
What is a Medical Eye Exam?
A medical eye exam is a comprehensive examination of your eyes conducted by an optometrist. This examination goes beyond a routine vision test and delves into the overall health of your eyes. During a medical eye exam, various tests will be performed to assess your visual acuity, peripheral vision, eye movement, and the health of your eye structures.
Medical eye exams can detect early signs of eye conditions that may not present noticeable symptoms in their initial stages. By diagnosing these conditions early, you have a greater chance of successful treatment and preventing further deterioration of your vision.
Medical eye exams can also identify underlying health conditions that may manifest in your eyes, providing an opportunity for early intervention and management.
Common Conditions Detected During a Medical Eye Exam
During a medical eye exam, several common eye conditions can be detected, even before noticeable symptoms occur. One such condition is age-related macular degeneration (AMD), which affects the central part of the retina responsible for sharp, central vision. By examining the retina, your optometrist can identify early signs of AMD and recommend appropriate treatment to slow its progression.
Another condition that can be detected during a medical eye exam is cataracts. Cataracts occur when the lens of your eye becomes cloudy, leading to blurred vision. Through a comprehensive examination, your eye doctor can assess the severity of your cataracts and recommend the most suitable treatment option, which may include surgery to remove the cloudy lens.
Hypertension is a common health condition that can have serious consequences if left untreated. The health of your eyes can provide valuable insights into your cardiovascular health. During a medical eye exam, an optometrist can observe changes in the blood vessels of your retina, such as narrowing or leaking. These changes can indicate underlying hypertension.

When it comes to maintaining your eye health, regular check-ups and screenings play a crucial role. One such screening method that has revolutionized the field of optometry is retinal imaging testing. This non-invasive procedure allows optometrists to capture detailed images of the retina, providing valuable insights into the overall health of your eyes.
The Importance of Retinal Imaging Testing
By examining the retina, which is the thin layer of tissue at the back of your eye responsible for capturing light and transmitting visual signals to the brain, optometrists can gain valuable insights into your eye health. Retinal imaging testing allows for the early detection of various eye conditions even before noticeable symptoms occur. This early detection is crucial as it enables prompt treatment and intervention, potentially preventing irreversible vision loss.
Advanced Retinal Imaging Technology
Retinal imaging testing has been made possible by the advancements in technology, specifically Optical Coherence Tomography (OCT) and Optos imaging. OCT is a non-invasive imaging technique that uses light waves to capture high-resolution cross-sectional images of the retina. It provides detailed information about the layers of the retina, helping eye doctors identify and monitor various eye conditions.
Optos imaging utilizes ultra-widefield retinal technology to capture a panoramic image of the retina. This technology allows for a more comprehensive view of the retina, including the periphery. Dilating drops are not necessary with Optos, making the process more convenient for patients.

Every patient is different and so are their eyes. This means that there need to be different types of contact lenses to suit each individual. Some patients have corneal abnormalities which mean that conventional lenses won’t sit comfortably on the surface of their eyes, while others suffer from eye conditions that mean normal contact lenses won’t be comfortable or could irritate their eyes.
As you may have guessed from the name, specialty contact lenses are unconventional contacts that are designed for patients that regular contacts might not be suitable. Here are some of the main types of speciality contact lenses and who they are recommended for.
Who might be a good patient for specialty contact lenses?
Some of the patients that might benefit from specialty contact lenses include those who:
Have been diagnosed with dry eye syndrome
Have corneal scarring
Have been diagnosed with keratoconus, a condition characterized by the bulging of the cornea
Suffer from strabismus, a condition where the patient has an eye that turns in or out relative to the other
Have suffered an injury to the eye
Suffer from a peripheral corneal thinning disorder
Are intolerant to other types of lenses
Your eye doctor or contact lens provider will be able to tell you if you need specialty contact lenses and if so, which lenses would be best based on your individual requirements.

If you find it difficult to tell colors apart, you may be color blind. Color blindness, or color deficiency, is estimated to affect around 8% of men and about 1% of women, but for those affected, it can significantly impact the quality of their day-to-day life. Contrary to popular belief, being color blind doesn’t mean that you can’t see any color at all. Instead, patients simply struggle to differentiate between certain colors. The vast majority of people who are color blind find it impossible to tell the difference between varying shades of red and green. You may hear this referred to as red-green color deficiency. However, this doesn’t only mean that they mix up red and green. They can also mix up colors that have some green or red light as part of their whole colors, for example purple and blue. This is because they are unable to see the red light that forms part of the color purple.
As you can probably imagine, this type of visual impairment can be a problem for things like traffic lights, taking medications and even looking at signs and directions. For example, someone who is color blind may find that the green on a traffic light may appear white or even blue.
InfantSEE
Your baby’s vision develops quickly during the first year of life and plays an important role in how they learn, move, and interact with the world. Even when a baby’s eyes appear healthy, certain vision or eye health concerns may not be obvious without a comprehensive infant eye assessment. InfantSEE is designed to help identify potential concerns early, giving parents peace of mind and helping children start life with the clearest, healthiest vision possible.
What Is InfantSEE?
InfantSEE is a program that helps parents access an early, comprehensive eye and vision assessment for babies between 6 and 12 months of age. It is designed to support healthy visual development by giving us an opportunity to check for early signs of vision or eye health concerns during a critical stage of growth.
The assessment is provided at no cost, making early eye care more accessible for families who want to be proactive about their baby’s vision.
The Importance of Early Vision Care
Many parents are surprised to learn that babies can have vision or eye health issues even before they are old enough to talk or read an eye chart. An infant may still track faces, reach for toys, or appear visually engaged while having an underlying concern that needs attention.
Early eye care can help detect signs of:
Eye alignment problems, such as crossed or turned eyes
Significant nearsightedness, farsightedness, or astigmatism
Eye movement or focusing concerns
Amblyopia risk factors, often called lazy eye
Signs of eye health conditions that may need monitoring or treatment
Finding these concerns early can make treatment more effective and may help support long-term visual development.

Eyelid hygiene is an essential aspect of maintaining optimal eye health. Your eyes are sensitive organs that require proper care and attention. Neglecting eyelid hygiene can lead to various problems, including dry eye.
Recognizing the Symptoms of Eyelid Problems
It is crucial to recognize the symptoms of eyelid problems to seek timely treatment and prevent further complications. Common symptoms of eyelid issues include redness, swelling, itching, irritation, crusting or scaling of the eyelids, sensitivity to light, and a sensation of something in the eye.
The Importance of Eyelid Hygiene in Maintaining Eye Health
Maintaining proper eyelid hygiene is essential for overall eye health. Regularly cleaning your eyelids helps remove debris, bacteria, and excess oil, preventing infections and inflammation. It also promotes the proper functioning of the meibomian glands, ensuring an adequate supply of tears to keep your eyes moisturized. By incorporating eyelid hygiene into your daily routine, you can significantly reduce the risk of developing dry eye and other eye-related problems.

Ray-Ban has long been recognized as a leader in timeless style, but now the brand is taking a bold step into the future. In collaboration with Meta, Ray-Ban has introduced a groundbreaking innovation - Ray-Ban Meta Glasses. These glasses are a fusion of iconic design and next-generation technology that allows you to capture, share, and stay connected like never before.
What Are Ray-Ban Meta Glasses?
Ray-Ban Meta Glasses go beyond vision correction or sun protection - they seamlessly integrate a camera, speakers, and voice-activated AI assistance, allowing users to capture, share, and interact hands-free. With their classic Ray-Ban frames, these glasses look just like traditional eyewear, but they’re packed with cutting-edge features hidden in plain sight.
Key Features and Technology
Built-in Cameras: Capture photos and videos instantly with a simple voice command or tap on the frame. The dual 12MP cameras allow for high-quality media with depth and detail.
Open-Ear Audio: Discreet speakers positioned near your ears provide clear sound without blocking ambient noise, letting you listen to music, take calls, or hear notifications seamlessly.
Meta AI Integration: Access Meta’s AI assistant through voice commands. Ask questions, control your device, or get updates - all without taking your phone out.
Live Streaming and Sharing: Stream directly to social media platforms like Instagram and Facebook in real time, making it easy to share your perspective with your audience.
Touch and Voice Controls: Intuitive touch-sensitive temples and responsive voice commands give you full control over your smart features.
Transitions® Lenses Option: Enjoy lenses that automatically adapt to changing light conditions for optimal comfort both indoors and outdoors.






